EDMONTON - People associate Dr. Dawn Davies with death.
As Edmonton's only palliative care doctor for children, Davies' job title can frighten family doctors and parents who may believe death and hopelessness are her companions.
"No physician wants to think their patient is going to die," Davies says. "Doctors don't want to make referrals because they don't want families to give up hope."
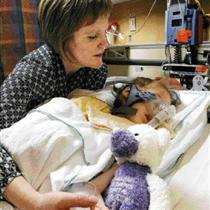
 Dr. Dawn Davies, Edmonton's only palliative care doctor for children, tends to five-year-old Kaitlyn Pas at University of Alberta Hospital. Kaitlyn, who has the most severe form of spinal muscular atrophy, lives a full life with school lessons and family picnics.Larry Wong, the Journal |
All of her patients have life-limiting or life-threatening illnesses such as cancer, heart disease, cystic fibrosis, multiple sclerosis and spinal muscle atrophy.
Some deem her career depressing and at odds with the medical philosophy to heal, but Davies sees it very differently.
"It's very life-affirming," says Davies, one of only about 10 pediatric palliative care doctors in Canada and the powerhouse behind a plan to create the first Canadian one-year training program in the specialty.
"You see people in these incredible situations and it's something about the capacity of human beings to survive."
For most people, she says, the term "palliative" equals "death." That's not always the case in her practice, which takes her and her team of bereavement counsellors and nurses into cancer clinics, intensive care units, doctor's offices and people's homes.
She generally sees between 30 and 50 families annually. While half of her patients die each year, others -- like babies with congenital heart disease who get transplants, or children with less severe forms of cystic fibrosis or multiple sclerosis -- can live into adulthood.
While under her care, Davies helps manage their pain and prepare families for the possibility of death. But more needs to be done in Canada to help these young patients, she believes.
Existing palliative programs already do a stellar job of caring for people with cancer and the elderly. Capital Health, for instance, is leading the world by giving access to palliative care to more than 80 to 85 per cent of cancer patients in the region, says Dr. Eduardo Bruera, who helped set up Edmonton's palliative program in 1995 and now works at the M.D. Anderson Cancer Centre in Houston, Tex.
Davies says cancer doctors have a lot of experience with death and are more open to referring patients to her when treatments fail.
With other diseases, the decision to seek palliative care is not as clear.
"When is the right time to involve us?" Davies says. "Most doctors think, 'It's too soon, it's too soon, it's too soon.' And then, it's too late."
A study published in June's Archives of Pediatric and Adolescent Medicine journal found that in 2002, only five to 12 per cent of children who could benefit from palliative care actually received services from eight dedicated pediatric palliative care programs in Canada. That means up to 95 per cent of dying children are not being helped by palliative doctors.
Instead, family doctors -- with little training in pain management and varying comfort levels in dealing with life-and-death issues -- try their best, says Davies, one of the study's authors.
"I don't think there are kids who need more help than kids who are dying," says Davies, whose proposal for a formal, one-year training program is supported by all of Canada's pediatric palliative programs. "These are the families who have the highest level of needs, living with that uncertainty and making difficult decisions."
Right now, pediatricians who want to improve their bedside training with dying children need to cobble together various funding sources, then head to children's hospitals in Boston and Sydney, Australia, as Davies did.
She began working in Edmonton in 1999.
Unlike adult palliative doctors, who tend to meet their patients in the last two to three months of life, Davies and her team step in as early as possible, sometimes meeting families before they give birth to talk about their baby's dangerous genetic disorder. She teaches them how to prepare their minds and homes for a child threatened by disease.
As the children grow, every effort is made to keep them in their homes where they may need IV morphine to dull the pain, wheelchair ramps, oxygen masks to aid weakening lungs, feeding and suction tubes for those unable to swallow or suck. Davies visits and adjusts medicine dosages; more often, home care nurses help with day-to-day activities, calling the doctor when the pain worsens or death's shadow comes close.
By providing grievance counsellors, Davies also gives parents an outlet to talk about the possibility their child may not live to adulthood. Parents learn it's normal to think about funeral plans. They feel liberated to talk openly about how a sick child can be a burden on the marriage and siblings.
"Nothing makes it better when your child has died, but families tell me (with palliative services) you feel less alone," Davies says. "It's not like we can make it all better. We totally can't, but we can help alleviate symptoms."
Because she's the only palliative doctor serving kids in northern Alberta, Davies relies on family doctors and dedicated home-care nurses in remote areas to care for her patients and to phone her for help.
Pediatric palliative care is a relatively new field which developed in the 1990s, two decades after hospital-based palliative care wards for adults opened in Canada for the dying parents of baby boomers. Davies believes care for kids lagged behind adults because many thought the nervous system of premature babies wasn't developed enough to cause pain. Even if babies could feel pain -- say, undergoing circumcision without anesthetic -- the medical community commonly thought the pain was short-lived and forgotten.
Subsequent research in the 1990s, and Davies' own experiences as a pediatric oncology nurse in the 1980s, debunked that. Davies saw too many kids crying, wanting to be at home, but dying in a lot of pain in hospital wards.
Back then, most cancer doctors didn't have a lot of training in pain management so they learned through trial and error, she says. The errors often showed up in children's tears.
As a palliative care doctor, she tackles issues that make others uncomfortable -- chief among them are the do-not-resuscitate type of orders. Parents and family doctors sometimes avoid these discussions, believing a choice implies a wish to hasten death.
In fact, such conversations are intimate and extremely privileged, says Deb
DeVlaming, a nurse who made palliative home visits for many years.
"It's a real honour to be part of a child's life," says DeVlaming, who now works to develop policies for Home Care Childrens Services. "I find it amazing, the capability of families to be able to care for loved ones and to learn what they never thought they could learn. They find the strength within themselves and it's remarkable to be able to witness that."
Now, following an agreement made by Canada's 17 medical schools, all medical students are to be trained in basic palliative medicine by 2008. Most of that training focuses on cancer and adult patients, but Davies has already seen a change in attitude and awareness since the new curriculum has been rolled out at the University of Alberta in the last few years.
More pediatric residents from the U of A are choosing to do elective work under her guidance. She also regularly speaks to medical classes on pain and death and comfort care.
Davies is able to teach future doctors when a child dying of cancer may need radiation treatment, not as a potential cure but to shrink tumours compressing the spinal cord and causing paralysis or extreme pain.
She can describe how some children who have lost limbs may need an epidural to decrease phantom pain, and explain how an epidural can also help a child with cystic fibrosis who coughs and fractures ribs.
In some cases, invasive surgery to implant a feeding tube is the right thing to do -- even though many family doctors will resist such procedures on kids who have already been poked and prodded many times, and who will ultim-ately die anyway.
For Davies, it is all part of helping families make choices that are best for them and their child.
"It's not about doing nothing and giving up, and that's what people often infer," Davies says.
"There is always more we can do."
jsinnema@thejournal.canwest.com